Scrotal Ultrasound (Testicular Ultrasound)
For Appointments Call: 786-332-4106 Miami 954-893-3811 Broward
Scrotal Ultrasound (Testicular
Ultrasound)
- What is Ultrasound Imaging of the Scrotum?
- What are some common uses of the procedure?
- How should I prepare?
- What does the equipment look like?
- How does the procedure work?
- How is the procedure performed?
- What will I experience during and after the procedure?
- Who interprets the results and how do I get them?
- What are the benefits vs. risks?
- What are the limitations of Scrotal Ultrasound Imaging?
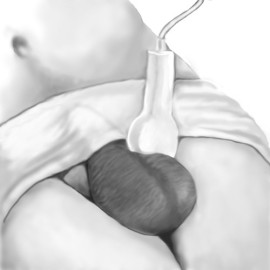
What is Ultrasound Imaging of the Scrotum?
Ultrasound imaging of the scrotum provides pictures of the testicles and the surrounding tissues of a man or a boy.
Ultrasound imaging, also called ultrasound scanning or sonography, involves the use of a small transducer (probe) and ultrasound gel to expose the body to high-frequency sound waves. Ultrasound is safe and painless, and produces pictures of the inside of the body using sound waves. Ultrasound examinations do not use ionizing radiation (as used in x-rays). Because ultrasound images are captured in real-time, they can show the structure and movement of the body's internal organs, as well as blood flowing through blood vessels.
Ultrasound imaging is a noninvasive medical test that helps physicians diagnose and treat medical conditions.
What are some common uses of the procedure?
Ultrasound imaging of the scrotum is the primary imaging method used to evaluate disorders of the testicles, epididymis (a tube immediately next to the testes that collects sperm made by the testicles) and scrotum.
This study is typically used to:
- Determine whether a mass in the scrotum felt by the patient or doctor is cystic or solid.
- Diagnose results of trauma to the scrotal area.
- Diagnose causes of testicular pain or swelling such as inflammation or torsion.
- Evaluate the cause of infertility such as varicocele.
- Look for the location of undescended testis.
Ultrasound is also a valuable tool for evaluating the epididymis and the prostate.
A sudden onset of pain in the scrotum should be taken very seriously. The most common cause of scrotal pain is epididymitis, an inflammation of the epididymis. It is treatable with antibiotics. If left untreated, this condition can lead to an abscess or loss of blood flow to the testicles.
Ultrasound can often detect an absent or undescended testicle as well. It is estimated that approximately three percent of full-term baby boys have undescended testicles. The testicle normally migrates from the abdomen, down the inguinal canal and then into the usual position in the scrotal sac. If it is not present in the scrotal sac, it may have stopped on its way and lie in the inguinal canal, in which case the ultrasound examination will often see it. If it has not left the abdominal cavity, it may not be seen by sonography. If a testicle is not detected, a urologist may be consulted in order to decide whether additional imaging such as an MRI is needed to determine its location. If the testicle is found to be in the inguinal canal, it can be moved into the scrotum. If left in the abdomen too long, it may become cancerous and may need to be removed.
Ultrasound can identify testicular torsion, the twisting of the spermatic cord that contains the vessels that supply blood to the scrotum. Caused by abnormally loose attachments of tissues that are formed during the fetal development, torsion commonly appears during adolescence, and less often in the neonatal period, and is very painful. Torsion requires immediate surgery to avoid permanent damage to the testes.
Ultrasound also can be used to locate and evaluate masses (lumps or tumors) in the testicle or scrotum. Collections of fluid and abnormalities of the blood vessels may appear as masses and can be assessed by ultrasound. Masses, both outside and within the testicles may be benign or malignant and should be evaluated as soon as they are detected.
How should I prepare?
You should wear comfortable, loose-fitting clothing for your ultrasound exam. You may need to remove all clothing and jewelry in the area to be examined.
You may be asked to wear a gown during the procedure.
No other preparation is required.
What does the equipment look like?
Ultrasound scanners consist of a console containing a computer and electronics, a video display screen and a transducer that is used to do the scanning. The transducer is a small hand-held device that resembles a microphone, attached to the scanner by a cord. The transducer sends out inaudible high frequency sound waves into the body and then listens for the returning echoes from the tissues in the body. The principles are similar to sonar used by boats and submarines.
The ultrasound image is immediately visible on a video display screen that looks like a computer or television monitor. The image is created based on the amplitude (loudness), frequency (pitch) and time it takes for the ultrasound signal to return from the area of the patient being examined to the transducer, as well as the composition of body tissue through which and the type of body structure the sound travels through.
In order to perform a scrotal sonogram, most commonly a linear small parts transducer is used.
How does the procedure work?
Ultrasound imaging is based on the same principles involved in the sonar used by bats, ships and fishermen. When a sound wave strikes an object, it bounces back, or echoes. By measuring these echo waves, it is possible to determine how far away the object is and its size, shape and consistency (whether the object is solid or filled with fluid).
In medicine, ultrasound is used to detect changes in appearance of organs, tissues, and vessels or detect abnormal masses, such as tumors.
In an ultrasound examination, a transducer both sends the sound waves and receives the echoing waves. When the transducer is pressed against the skin, it directs small pulses of inaudible, high-frequency sound waves into the body. As the sound waves bounce off of internal organs, fluids and tissues, the sensitive microphone in the transducer records tiny changes in the sound's pitch and direction. These signature waves are instantly measured and displayed by a computer, which in turn creates a real-time picture on the monitor. One or more frames of the moving pictures are typically captured as still images. Small loops of the moving “real time” images may also be saved.
How is the procedure performed?
For most ultrasound exams, the patient is positioned lying face-up on an examination table that can be tilted or moved.
A clear water-based gel is applied to the area of the body being studied to help the transducer make secure contact with the body and eliminate air pockets between the transducer and the skin that can block the sound waves from passing into your body. The sonographer (ultrasound technologist) or radiologist then presses the transducer firmly against the skin in various locations, sweeping over the area of interest or angling the sound beam from a farther location to see an area of concern better.
When the examination is complete, the patient may be asked to dress and wait while the ultrasound images are reviewed.
This ultrasound examination is usually completed within 15 to 30 minutes, though sometimes more time is necessary.
What will I experience during and after the procedure?
Ultrasound examinations are painless, fast and easily tolerated by most patients.
After you are positioned on the examination table, the radiologist or sonographer will apply some warm water-based gel on your skin and then place the transducer firmly against your body, moving it back and forth over the area of interest until the desired images are captured. There is usually no discomfort from pressure as the transducer is pressed against the area being examined.
If scanning is performed over an area of tenderness, you may feel pressure or minor pain from the transducer.
Once the imaging is complete, the clear ultrasound gel will be wiped off your skin.
After an ultrasound examination, you should be able to resume your normal activities immediately.
Who interprets the results and how do I get them?
A radiologist, a physician specifically trained to supervise and interpret radiology examinations, will analyze the images and send a signed report to your primary care physician, or to the physician or other healthcare provider who referred you for the exam, who will share the results with you. In some cases the radiologist may discuss results with you at the conclusion of your examination.
Follow-up examinations may be necessary, and your doctor will explain the reason why another exam is needed. Sometimes a follow-up exam is done because a suspicious or questionable finding needs clarification with additional views or a special imaging technique. A follow-up examination may be necessary so that any change in a known abnormality can be monitored over time. Follow-up examinations are sometimes the best way to see if treatment is working or if an abnormality is stable over time.
What are the benefits vs. risks?
Benefits
- Most ultrasound scanning is noninvasive (no needles or injections).
- Occasionally, an ultrasound exam may be temporarily uncomfortable, but it is almost never painful.
- Ultrasound is widely available, easy-to-use and less expensive than other imaging methods.
- Ultrasound imaging is extremely safe and does not use any ionizing radiation.
- Ultrasound scanning gives a clear picture of soft tissues that do not show up well on x-ray images.
- Ultrasound provides real-time imaging, making it a good tool for guiding minimally invasive procedures such as needle biopsies and needle aspiration.
Risks
- For standard diagnostic ultrasound, there are no known harmful effects on humans.
What are the limitations of Scrotal Ultrasound Imaging?
Ultrasound of the scrotum is helpful for finding abnormalities such as masses in the scrotum or testicles. However, it does not always permit an exact diagnosis (i.e., the exact type of tissue a mass is composed of, especially when the mass is solid). Blood flow images of the testicles are not always reliable in determining if the blood supply to a testicle has twisted. When searching for an absent testicle, ultrasound may not be able to find it if it is located in the abdomen because gas filled bowel loops may block the view.